Recently, the Obama administration, along with the U.S. Department of Health and Human Services and the Food and Drug Administration, has spotlighted the emergence of a prescription drug and heroin use epidemic in the United States. According to a 2010 infographic produced by the National Institute on Drug Abuse, an estimated 8.76 million Americans had reportedly abused their prescriptions, 81.6 percent of whom had been prescribed these drugs by a doctor. In an effort to combat opioid abuse, the Tufts School of Dental Medicine has joined forces with other Massachusetts dental schools to introduce a curriculum focusing on preventing opioid addictions in patients.
According to a presentation emailed to the Daily by Dr. Kulich, a professor at the dental school who specializes in the psychological assessment of chronic pain, drug overdose has become a significant cause for emergency medical conditions which have led to 2.5 million visits in 2011, 1.4 million of which are related to prescriptive drugs. The new curriculum will cater towards informing future dentists about the epidemic in efforts to curb patient addiction.
"It's a curriculum that addresses pain and addresses risks for substance use,” Kulich said. “The current program [at dental and medical schools] everywhere certainly could use improvement…The goal is to improve all of them.”
Kulich's presentation outlines the new curriculum's “core competencies” for future dentists, focusing on effective and healthy management of pain. The program is a part of the effort of the Working Group on Dental Education on Prescription Drug Misuse initiated by Governor of Massachusetts Charlie Baker, based on the joined forces of three major dental schools in Massachusetts – Boston University, Harvard and Tufts, as well as support from Massachusetts Dental Society. The working group was established in November 2015 with the direct purpose of combatting current problems in pain control and raising awareness among professionals to limit the prescription of opioid drugs.
Unfortunately, opioid abuse in the United States is an incredibly widespread problem. According to a Feb. 13 article in Modern Healthcare magazine, the United States was responsible for 99 percent of hydrocodone and 81 percent of oxycodone sales globally in 2012. Hydrocodone, more commonly known as Vicodin, and oxycodone, such as Percocet, are commonly prescribed by doctors and dentists following oral surgery. In 2013, as many as 22,767 lives have been taken by prescriptive drug overdoses, 71.3 percent of which are related to opioid drugs. Drug overdose is also a significant cause for emergency medical conditions, leading to 2.5 million visits in 2011, with more than 1.4 million related to prescriptive drugs, according to Kulich.
According to the Modern Healthcare article, doctors have been unwittingly contributing to the widespread addictive behaviors throughout the country, often with the intention of relieving their patients' pain. Opioids that are frequently prescribed include morphine, methadone, hydromorphone and fentanyl.
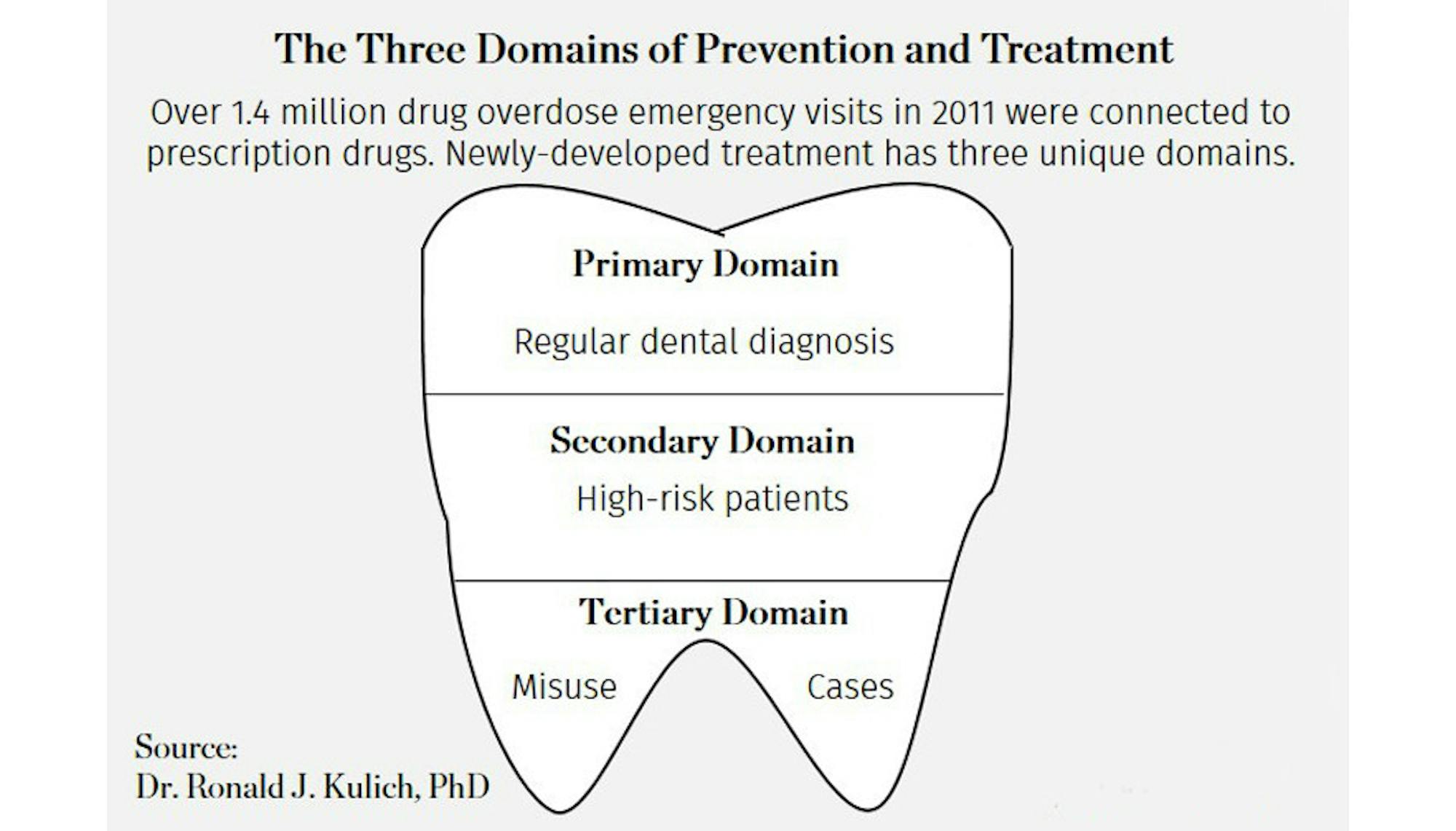
The new dental school curriculum offers “core competencies” which entail three major parts: the primary, secondary and tertiary prevention domains, with each focusing on distinct aspects of patient treatment. The primary domain deals with assessing the necessity and limiting prescription upon screening of patients and diagnosis, the secondary domain is concerned with effective communication and with cautionary treatment for high-risk patients and the tertiary domain with managing patients already troubled with prescriptive drug abuse. In other words, the primary domain applies in regular dental diagnosis, the second narrows its focus to high-risk patients and the third works with misusing patients directly.
Additionally, according to a Feb. 11 article in the Boston Globe, the program will ensure that future dentists not only evaluate their patients' pain but also their risk for opioid abuse.
"Kulich...said because dentists are constantly addressing pain issues, they have a potentially influential role in detecting and helping troubled patients," the article said.
As a co-chair in Baker’s working group, Kulich has been promoting the curriculum and communicating it with the dental school faculty. According to Kulich, professionals around Massachusetts and the globe, including experts from Saudi Arabia and France, will also participate in weekly sessions of the Inter-Professional Facial Pain and Headache Rounds, which give dental students firsthand information on new directions in the pain management field.
Senior Ratan Marwah, a prospective student in the dental school class of 2020, said that appropriate pain control practices are critical to dentistry.
"The knowledge of all this, informing the patient and the students themselves learning about this is very important," he said. "I think [the new curriculum is] a good thing."
Another student who looks forward to being a dentist, first-year Nelson Zhang, looks at the practices at a more individual level.
“Dentistry is like a fine art," Zhang said. "It really depends on each artist per se and how he handles things, on the level of education and generally the amount of skill that person has.”
While Zhang doesn’t think that dentists are solely to blame for the opioid crisis, he doesn’t put the responsibility on the shoulders of patients either. He explained that many problems stem from the fact that different medical institutions often don't communicate with one another.
“I've been through enough situations in which my friends try to abuse a prescription drug…which is [a] problem nowadays,” he said. "[If] even one healthcare institution determines a certain patient as unsuitable for an addictive medication, he or she will be able to acquire it from another doctor’s hands [because] nothing is linked. It's a more widespread issue, mainly in doctor to patient communication, patient intentions and hospital communication or clinic communication."
The new curriculum hopes to address communication between doctors and patients by making the doctors aware of their responsibility to inform their patients of the potential threat of drug misuse, which will equip the population with proper pain management knowledge on a basic level.
Tufts Dental School joins the fight against opioid abuse